Effects of COVID measures not clear enough
- General
- Healthcare
Long-term crisis
The Dutch Safety Board’s second research report looks at the period after the relatively calm summer of 2020, during which the Netherlands faced a new surge in coronavirus infections and hospital admissions. This was when the general public started to realise that the coronavirus pandemic was not over yet, and that it would be a long-term crisis. In the autumn of 2020 and the winter of 2020-2021, the Cabinet introduced far-reaching measures to curb the spread of the virus. These included a facemask requirement, the closure of primary and secondary schools, and a curfew. Little was known at the time about the effects these measures would have, an uncertainty that persists to this day as a result of insufficient monitoring and evaluation. The Board recommends that more knowledge be collected about the effects of the measures, as this would allow the Cabinet to make better-informed decisions in the event of coronavirus resurgences or future pandemics.
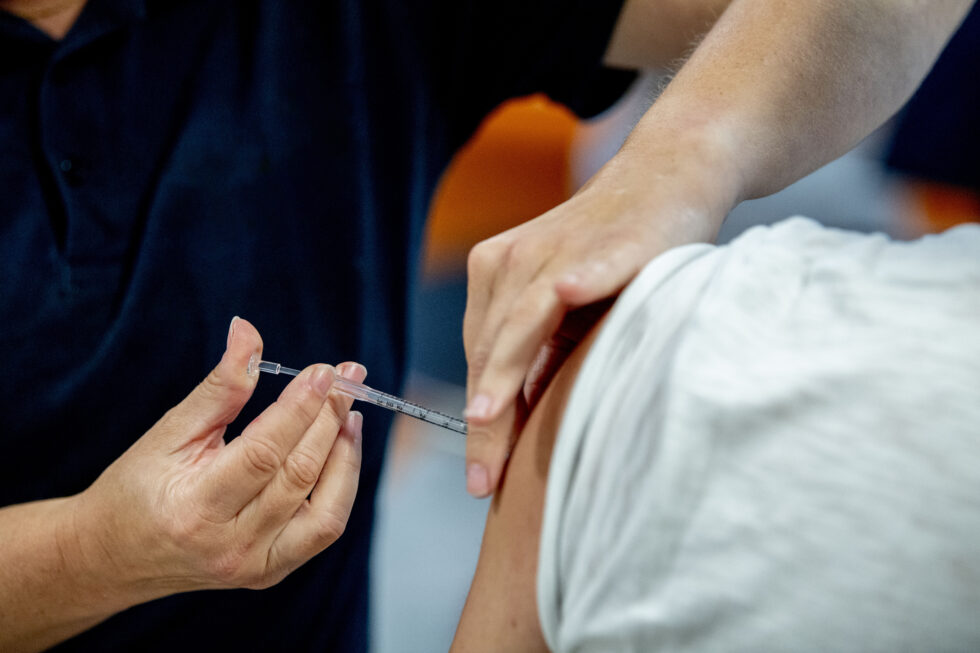
Vaccination programme
European cooperation enabled effective vaccines to be developed and made available within an unprecedented timeframe. The Netherlands played an active role in this process. When the vaccination campaign started in early January 2021, expectations were high. However, vaccines remained in short supply for several months, whereupon it became necessary to prioritize. The Dutch Health Council advised the Cabinet to vaccinate the most vulnerable groups first: the elderly and people who were at risk due to medical reasons. The Cabinet chose to deviate from this advice to some extent. Healthcare workers in long-term care were vaccinated first, followed by people the government classified as vulnerable to the virus due to medical reasons. The latter group, however, did not include all at-risk groups. As a result, at-risk groups that were not eligible for early vaccination felt unfairly disadvantaged. In the end, they were vaccinated months later than originally planned. After a hesitant start, the vaccination campaign started to pick up steam, and by June 2021 a large proportion of the population was vaccinated.
Division of roles and scenarios
Looking at this second period of the COVID-19 crisis, the Board observes the same patterns it saw in the first part of its investigation. In its first sub-report, the Board concluded that the division of roles – the Cabinet as decision-maker and the experts as advisers – was not always clear. The Board notes that this was also the case during the decision-making process regarding the facemask requirement. Initially, the Cabinet followed the Outbreak Management Team’s (OMT) recommendation not to institute a facemask requirement. Only later, as a result of political pressure, did the Cabinet change its view on the matter. The OMT did not always adhere to its formal role at times, for instance when it allowed the scarcity of facemasks to become a factor in its negative recommendation regarding facemask requirement.
In addition, the Board again notes that the Cabinet did not sufficiently consider a variety of possible scenarios. For instance, in preparing the vaccination campaign, the Cabinet assumed that the vaccine would be administered by general practitioners. All preparations were geared towards that scenario. When it eventually became apparent that the first vaccine to become available was not suitable for distribution through general practitioners, a last-minute switch to large-scale vaccination by the Municipal Health Departments (GGDs) was required. This put significant pressure on the Municipal Health Departments (GGDs) to set up large vaccination sites in a short timespan.
